Explore the tool and find trusted vasculitis care wherever you live.
Vasculitis Types
About Polymyalgia Rheumatica
Last Updated on February 5, 2024
Polymyalgia rheumatica (PMR) is a rare inflammatory disease that affects older adults, causing widespread muscle pain and stiffness, especially around the shoulders and hips. Most people who develop PMR are in their 60s or 70s. PMR is closely linked with giant cell arteritis (GCA), a type of vasculitis characterized by inflammation of the arteries in the head (temples) and of the aorta, resulting in headaches and vision problems. Left untreated, GCA can lead to blindness and stroke. The two diseases can occur at the same time in the same person. Approximately 15 percent to 20 percent of people with PMR will develop GCA, while about half of patients with GCA also have symptoms of PMR.

Quick Facts

Number of cases worldwide unknown

50 per 100,00 US cases per year

More common in older adults with the average onset age is 70

Extremely rare in people under 50

2 times more likely in females than males

More common in people of northern European and Scandinavian descent
Polymyalgia rheumatica (PMR) is a rare inflammatory disease that affects older adults, causing widespread muscle pain and stiffness, especially around the shoulders and hips. Most people who develop PMR are in their 60s or 70s. PMR is closely linked with giant cell arteritis (GCA), a type of vasculitis characterized by inflammation of the arteries in the head (temples) and of the aorta, resulting in headaches and vision problems. Left untreated, GCA can lead to blindness and stroke. The two diseases can occur at the same time in the same person. Approximately 15 percent to 20 percent of people with PMR will develop GCA, while about half of patients with GCA also have symptoms of PMR.
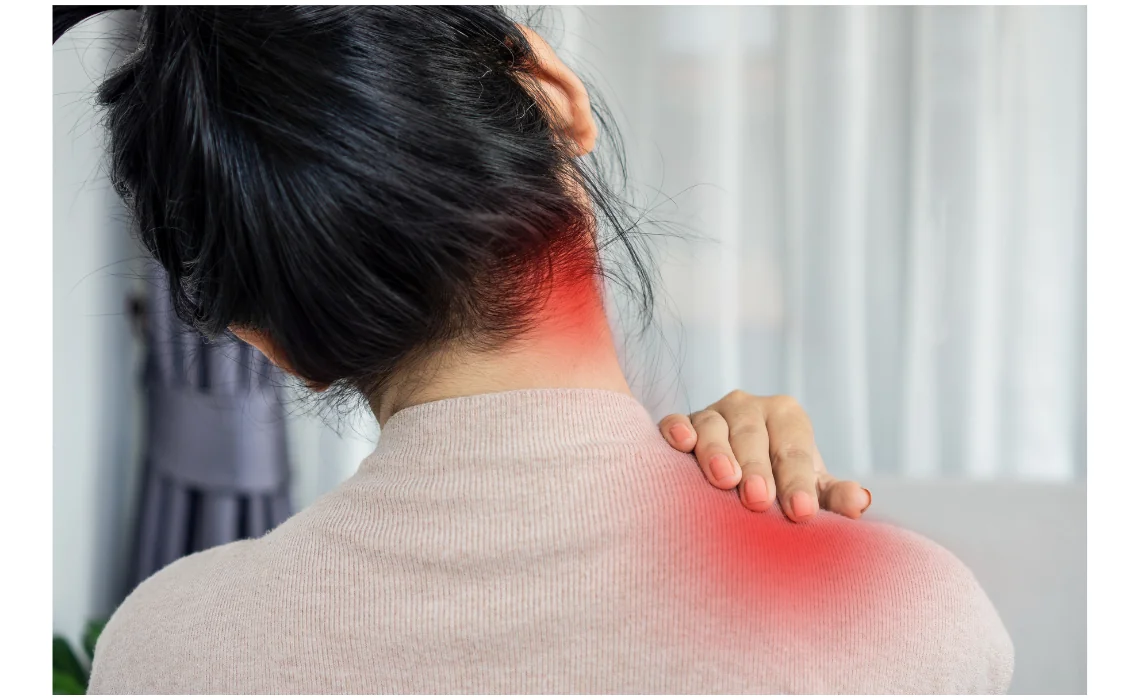
PMR primarily affects the shoulders, neck, hips, lower back, and thighs, with muscle pain and stiffness that is worse in the morning. As a systemic disease (affecting the whole body), PMR also causes flu-like symptoms such as fatigue and fever. Rarely, PMR causes inflammation of the body’s largest artery, the aorta. This can lead to a potentially life-threatening aortic aneurysm, an abnormal bulging of the weakened vessel that can burst.
The symptoms of PMR can come on suddenly, over a period of days or weeks. Glucocorticoid medications such as prednisone are prescribed to reduce inflammation and pain. Patients usually respond quickly, within 24 to 48 hours, but most need to remain on treatment for a year or more. The disease typically runs its course in one to five years. However, even with effective treatment, relapses can occur, so ongoing medical follow-up is essential.
Because of the disease association with GCA, it is important to see your doctor right away if you develop headaches, tenderness in the temples, changes in vision, jaw pain, or fever.
The exact cause of PMR is unknown. Like vasculitis, it is classified as an autoimmune disorder—a disease that occurs when the body’s natural defense system mistakenly attacks healthy tissue. Researchers believe genetics and environmental factors may play a role in the onset of PMR. Rarely, the disease occurs in an individual who has cancer. New cases of PMR often occur seasonally, suggesting that a virus may play a role in triggering the disease.
PMR is considered a common cause of aching and stiffness in older adults. The average age of patients is about 70, and PMR almost never affects people younger than 50. Women get PMR almost twice as often as men. PMR is the second-most common rheumatic disease after rheumatoid arthritis (RA).
In the United States, disease prevalence is estimated at 50 people per 100,000 per year, and it affects Caucasians more than any other ethnic group. Internationally, prevalence varies country by country. People of Northern European and Scandinavian descent have the highest risk of getting the disease.
For reasons that are not well-understood, PMR and GCA are considered linked inflammatory conditions that may occur together but affect different parts of the body. They are frequently discussed together because of their close association.
The symptoms of PMR often start suddenly and include pain, aching and stiffness in the shoulders, neck, upper arms, hips, lower back, and thighs. Symptoms are worse in the morning or after inactivity. Other common symptoms include:
- Low-grade fever
- Weight loss
- Loss of appetite
- Limited range of motion in joints
- Fatigue
- General flu-like feeling
Left untreated, PMR can interfere with mobility, making it difficult to perform daily activities such as dressing, bathing, combing hair, standing up from a couch and getting in and out of a car. Raising the arms over the head can be especially difficult. Very rarely, PMR can cause inflammation of the aorta, the artery which carries blood from the heart to the rest of the body. This can lead to a potentially life-threatening aortic aneurysm.
Serious complications of PMR can also occur when patients develop GCA, which causes narrowing of the arteries in the head and the temples, resulting in persistent headaches, scalp tenderness, and vision changes. Without treatment, GCA can result in stroke, blindness or aortic aneurysm.
There is no single test for diagnosing PMR, so your doctor will consider several factors including a detailed medical history, physical examination, laboratory tests, and less frequently, imaging studies. Your doctor will also look for symptoms and signs of GCA.
Part of the diagnosis is ruling out diseases that may cause similar symptoms such as RA, other forms of vasculitis, infections, other muscle diseases or cancer. To make an accurate diagnosis of PMR, the following tests may be ordered:
- Blood tests: Common tests include a complete blood cell count, erythrocyte sedimentation rate (ESR, or “sed rate”) and C-reactive protein (CRP) levels, which, when elevated, suggest inflammation.
- Imaging studies: Ultrasound or magnetic resonance imaging (MRI) may be used to detect inflammation in structures around the joints. Computed tomography angiography (CTA) or magnetic resonance angiography (MRA) may be needed for evaluation of the aorta and its main branches.
- Biopsy: If your doctor suspects inflammation of the blood vessels such as in GCA, you may undergo a biopsy. This involves surgical removal of a segment of an artery in the temple, which is sent to a laboratory and examined for signs of inflammation.
PMR is primarily treated with low doses of glucocorticoids to control inflammation and pain. Most patients experience symptom relief within a few days, at which time the dose may be gradually lowered. A maintenance dose is usually required for several months up to a few years. Higher doses may be prescribed for people with recurring headaches or other symptoms suggestive of GCA.
Researchers have been studying the effects of immunosuppressant drugs such as methotrexate in treating PMR, but results are not conclusive. On February 28, 2023, the U.S. Food and Drug Administration (FDA) approved sarilumab, a biologic drug, for the treatment of adults with PMR for whom glucocorticoids were inadequate or who could not tolerate a glucocorticoid taper. Biologic medications are complex proteins derived from living organisms; they target certain parts of the immune system to control inflammation.
In addition to medication, regular exercise is an important component of the treatment plan, especially low-impact activities such as walking, swimming, or riding a stationary bicycle. Physical therapy may be helpful in maintaining mobility and reducing discomfort.
Glucocorticoids carry the risk of serious side effects such as potential bone loss (osteoporosis), cataracts, glaucoma, and increased chance of infection, among others. Therefore, it’s important to see your doctor for regular checkups. Medications may be prescribed to offset side effects. Infection prevention is also very important. Talk to your doctor about getting vaccines (e.g., flu shot, pneumonia and/or shingles vaccination), which can reduce your risk of infection.
Even with effective treatment, relapses can occur with PMR. If your symptoms return or you develop new ones, report them to your doctor as soon as possible. Regular doctor visits and ongoing monitoring are important in detecting relapses and preventing complications.
Effective treatment of PMR may require the coordinated efforts and ongoing care of a team of medical providers and specialists. In addition to a primary care provider, you may need to see the following specialists:
- Rheumatologist (joints, muscles, immune system)
- Ophthalmologist (eyes) or others
The best way to manage your disease is to actively partner with your health care providers. Get to know the members of the health care team. It may be helpful to keep a health care journal to track your medications, symptoms, test results and notes from doctor appointments in one place. To get the most out of your doctor visits, make a list of questions beforehand and bring along a supportive friend or family member if necessary to provide a second set of ears and take notes.
Remember, it’s up to you to be your own advocate. If you have concerns about your treatment plan, be sure to speak with your medical team. It’s always your right to seek a second opinion.
Living with a chronic disease such as PMR can be challenging at times. Fatigue, pain, emotional stress, and medication side effects can take a toll on your sense of well-being, affecting relationships, work, and other aspects of your daily life. Sharing your experience with family and friends, connecting with others through a support group, or talking with a mental health professional can help.
People with PMR typically respond well to treatment and most eventually recover entirely from the disease within one to five years. With appropriate treatment and regular follow-up care, individuals with PMR, and even those who develop GCA, can experience a normal and productive life.
Recently, it has been recognized that patients with PMR are at higher risk for atherosclerosis, or hardening of the arteries, although life expectancy overall does not appear to be affected.
- Learn more on the National Institutes of Health web page for Polymyalgia Rheumatica and Giant Cell Arteritis
- Check out this great resource, Maintaining movement, activity and exercise with PMR, from our friends at PMR/GCA UK. If you use this resource, please take a minute to provide helpful feedback to the authors. Just scan the link on the back cover to complete a brief questionnaire.
- Find even more helpful PMR & GCA resources from PMR/GCA UK at https://pmrgca.org.uk/information-and-advice/resources/
- Global Healthy Living Foundation Podcast Unpacking Polymyalgia Rheumatica: Expert and Patient Insights
- Learn PMR online resources from Global Healthy Living
Polymyalgia Rheumatica Videos
What You Need to Know About Sarilumab (Kevzara®) for PMR 2025
Research Insights: Investigating the causes of GCA and PMR 2022