Prednisone
About Steroids
The initial treatment for vasculitis frequently involves taking high doses of glucocorticoids (steroids) such as prednisone. Steroids quickly reduce inflammation, protecting vital organs; but they also have a lot of side effects. Learning what side effects to expect and being prepared with strategies to help minimize side effects can help you feel more in control as you navigate treatment.
Meet Sam (Steroids and Me)
Sam (steroids and me) is an online app designed to help people on their steroid journey. Built by doctors, scientists and patients, Sam provides free education and practical tips from experienced medical experts to equip you with the knowledge to manage side effects and work with your doctor toward a safe steroid taper.
Sam’s Journey Tracker enables you to record your mood, health concerns and side effects quickly, and as they happen, and easily share them with your doctor at your next appointment.
Key Takeaways
- Stopping your high-dose glucocorticoid (steroid) medication without tapering can be dangerous. Work with your healthcare provider to safely taper your steroid dose.
- Your chances of experiencing side effects is greater if you are on a high dose of steroids for a long period of time.
- Once the vasculitis inflammation is controlled and the risk of damage to vital organs has decreased, your healthcare provider will work with you to taper your dose of steroids.
- While vasculitis patients hope to be able to stop taking steroids completely, many find it necessary to remain on a low dose of steroids in order to control their vasculitis.
- There are medications that are designed to decrease the need for long-term steroid use and are relatively safer to take long-term for the treatment of vasculitis. Depending on what type of vasculitis you have, and your individual response to treatment, you may find that one of these medications can effectively control your vasculitis.

FAQs
Vasculitis is characterized by inflammation of the blood vessels. When blood vessels are inflamed, not as much blood can pass through them. Organs, such as the heart, lung, and kidneys, are damaged by the lack of oxygen and nutrients carried by the blood. The first goal in treating vasculitis is to control the inflammation as quickly as possible to protect your organs. This is done by suppressing the immune system which decreases the body’s inflammatory response.Steroids, such as prednisone and methylprednisolone, quickly and effectively decrease the inflammation and prevent further organ damage. Other vasculitis treatments can take months to reduce inflammation. By then, severe and sometimes life threatening organ damage has occurred.
Some people who have been diagnosed with vasculitis are able to stop taking steroids after a few months, but most will need some level of steroids for years, or even for the rest of their life, in order to achieve and maintain remission.
Remission, in vasculitis, refers to the period of time when the vasculitis inflammation is controlled and you are not experiencing active symptoms of the disease. This does not mean you will not experience any symptoms. The damage that was done while your vasculitis was active may still cause symptoms. You and your healthcare provider will work closely to craft a treatment plan that will help you achieve and maintain remission. You will also work with your healthcare provider to plan how you will monitor for flares (periods when your vasculitis becomes active again). Not everyone with vasculitis experiences flares.
Health care providers are very aware of the side effects associated with steroids. Their first goal is to protect your organs and save your life. They will then work with you to safely taper your steroid dose. The side effects of steroids are less severe at lower doses.
Want to learn more about remission and relapse?
Typically steroids, which mimic your body’s natural cortisol, are taken in one dose in the morning. This is to mimic the normal peak of cortisol levels in the morning.
If your doctor prescribes a split dose, meaning you take your steroid medication twice a day, you should take the first dose in the morning and the second dose in the late afternoon or early evening. Taking the second dose too close to bedtime may disrupt your sleep.
It is best to take your oral steroids with a meal to help minimize irritation to your gastrointestinal system.
Ask your doctor or pharmacist what to do in case of a missed dose.
If you have trouble swallowing pills, ask your doctor or pharmacist if there is a liquid form of the medication or if the pill can be safely crushed.
- It is important that you reduce your dose of steroids (called tapering) slowly and methodically following the plan outlined by your healthcare provider. Abruptly reducing or stopping steroids may result in a potentially fatal condition called adrenal insufficiency.
- Some people notice that the side effects they experienced while on high dose steroids such as anxiety, mood swings, pain and fatigue worsen temporarily during the tapering process. This temporary worsening of symptoms occurs most commonly during the first few days after a reduction in dosage.
- Work closely with your healthcare provider during the tapering process. Ask them what to expect and what symptoms are important for you to report to them. You may have to temporarily halt the tapering process, especially if your disease symptoms return.
- If you need surgery, discuss the need for perioperative (around the time of surgery) steroids with your surgeon and the clinician who is prescribing your steroids. Some patients who are on long-term steroid treatment need a dose of steroids before surgery to help counter the effects of adrenal suppression.
Want to learn more?
Read “When is perioperative steroid coverage necessary?”
Watch Risk of Corticosteroids: Adrenal Suppression – Pharmacology | Lecturio Nursing
- Know the Potential Side Effects Both you and your loved one need to know what side effects may occur so that you can do what you can to decrease the severity of side effects and know when you need to talk to your healthcare provider.
- Expect the Mood Changes One care partner described the effects of prednisone on their partner’s personality as “extending the extremes of their behavior.” The faults and flaws and imperfections that we all have may be harder for your loved one to control while they are taking steroids. When you add the stress of a life-changing diagnosis and the additional physical changes associated with vasculitis such as pain and fatigue to the mix, the personality changes you see in your loved one may be pronounced and upsetting to you and them. Try to remember that this is not forever. You and your loved one will both notice improvement once their body has adjusted to the dose of steroids they are on. As with most side effects associated with steroid treatment, the mood changes are most severe when beginning high-dose treatment and during tapering. Once your loved one has tapered down to a “maintenance” dose of steroids or is off of steroids completely, the mood changes associated with steroid treatment will subside.
- Take Care of Yourself Make some time in your day (even just a few minutes) for doing something just for yourself. Ask friends and family members to help. People want to help but often don’t know what to do. Suggest a specific task that would help lighten your load such as picking up a grocery order, taking care of a chore that your loved one normally handles but is unable to right now, or providing a meal.
- Educate your child about their vasculitis and their medications in an age-appropriate way. School-aged children should be included in discussions between you and their healthcare team. In many cases, vasculitis is a life-long illness and once your child turns 18, they will be the ones responsible for making healthcare decisions. The earlier you involve them and educate them the better.
- Make sure your child understands the dangers of abruptly stopping steroids. If your child is old enough to understand, educate them about the complications of stopping steroids without tapering such as steroid withdrawal, adrenal insufficiency, and adrenal crisis.
- Keep healthy snacks on hand. Steroids typically cause a marked increase in appetite. Keep plenty of nourishing, healthy, low-calorie snacks on hand. You may also talk with your child’s school about allowing them to bring snacks.
- Talk to your child’s teachers. Your child may experience mood changes, hyperactivity, and trouble concentrating. It is important for your child’s teachers to know that these changes are medication related.
Want to Learn More?
Steroids & Vasculitis
TAVNEOS® (avacopan) ASN Perspectives_Geetha
Pediatric Medications: What's available for childhood vasculitis
Vasculitis Medications for Children
Current Treatments for GPA and MPA including Avacopan
ACRVF Guidelines Conference: EGPA Breakout
ACR_VF Guidelines: GPA-MPA Breakout
ACRVF Guidelines Conf PAN Breakout
ACRVF Guidelines Conf GCA Breakout
ACR VF Guideline Langford Session 2
Introducing the 2021 ACR/VF Vasculitis Clinical Practice Guidelines Part 1
Introducing the 2021 ACR/VF Vasculitis Clinical Practice Guidelines Part 2: Q&A
Possible Side Effects
The list of possible side effects associated with long-term use of high-doses of glucocorticoids (steroids) is long, but most patients do not experience all or even most of these side effects. However, being aware of what side effects might occur is important for three reasons:
- There are steps you can take to help decrease the impact of some side effects.
- Knowing what to expect can make it easier to deal with the side effects.
- Familiarity with expected side effects can help you know when you need to discuss certain side effects with your healthcare provider
Possible Side Effects:
- Easily upset or angered
- Just don’t feel like yourself
- Increased anxiety
- Depression
- Hyperactivity
- Difficulty concentrating
- Irritability
- Restlessness
- Mood swings
- Euphoria (intense excitement or happiness)
Why does this happen?
It is the result of the effects that glucocorticoids (steroids) have on brain receptors, neurotransmitters, and hormones.
When are these effects most likely to be noticed?
- At the beginning of your treatment with high-dose steroids
- When tapering
- If your dose is increased after a taper
What can you do?
- Talk with your healthcare provider if the mood changes are severe. They may need to make changes to your treatment.
- Ask your healthcare provider about what mood changes to expect.
- Talk with your healthcare provider about taking medications to help with depression or anxiety if needed.
- Let your friends and family know what to expect and ask for their understanding.
- Avoid stressful situations as much as possible.
- Use strategies that can help lessen anxiety and depression such as mindfulness and meditation, weighted blankets, time in nature, exercise, avoiding or limiting alcohol (alcohol is a depressant), avoiding or limiting caffeine (can amp up anxiety), etc.
It Worked For Us
We asked people who are living with vasculitis their best tips for dealing with mood changes. Here are some of their responses:
- “Breathe in sloooowly. Breathe out. Rest assured, everything will be okay!”
- “Doing a calming activity I enjoy: coloring, crochet, journaling, playing music, etc.”
- “It’s best to find something to shift your focus! It’s okay to let it out but don’t let yourself get stuck.”
- “Remind yourself you’re human and it’s most likely the meds talking. Take a deep breath.”
- “Talk to someone and share your feelings.”
- “Good food and a movie or tv show you enjoy. Sometimes all you need is some time to yourself.”
Why does this happen?
Researchers believe sleep disturbances while on high doses of glucocorticoids (steroids) are related to the effects of higher levels of cortisol (fight or flight hormone) in the body.
What can you do?
- Some people find that they have extra energy while on steroids and this can help lessen the physical impact of getting less sleep.
- Talk with your healthcare provider about taking melatonin or chamomile.
- With your healthcare provider’s approval, take your entire dose of steroid medication in the morning.
- Steroids may give you extra energy, but avoid physical activity in the late evening which may make it more difficult for you to fall asleep.
- Stay on a sleep schedule and have a sleep routine. This can help signal to your brain that it is time to fall asleep.
- Get some sunlight in the morning to help regulate your sleep/wake cycle.
It Worked For Us
We asked people who are living with vasculitis their best tips for dealing with insomnia. Here are some of their responses:
- “Relaxing music, eye mask for sleep, tire the brain with tasks and hobbies.”
- “Massaging coconut oil on feet and scalp”
- “I take melatonin and take my steroids early in the day.”
- “Listening to podcasts has worked when I’m struggling to get to sleep”
- “Bed is for sleeping, stick to routine, weighted blanket”
- “Try to get extra sleep in the afternoons.”
- “Magnesium oil spray with lavender”
- “White noise! I listen to rain podcasts”
- “Take a warm bath before sleeping, get into the coziest pjs, and get a cozy blanket”
- “Theanine is really awesome & playing rain sounds”
- “Valerian root tea!”
- “Take the meds early in the day if possible, no caffeine, exercise, and then read.”
- “Magnesium & reducing screen time before bed”
- “Herbal tea”
*Check with your pharmacist or healthcare provider before using any supplements, including herbal supplements, as some may interfere with medications you are taking.
*Some people found it helpful to talk to their healthcare provider about getting a prescription for medications that helped calm them or helped them sleep. It is important to weigh the pro’s and con’s of taking these medications with your healthcare provider. Many of these medications increase your risk of falls, increase daytime drowsiness, and interact with other medications.
Possible Side Effects:
- Ruddy (red) complexion
- Fat redistribution to the upper back and midriff
- Round, puffy face sometimes referred to as moon face
All of these changes together are often referred to as having a cushingoid appearance which is a reference to the physical changes that are seen with Cushing’s Syndrome. Cushing syndrome occurs when tumors on the adrenals cause excess production of glucocorticoids (steroids), so the physical effects are similar to what is seen when someone is being treated with high doses of steroids.
Steps you can take to prevent appearance changes:
There is nothing you can do to prevent these changes. They occur to some degree in everyone who is treated with high doses of steroids. In most cases, people find that once their steroid dose is tapered to what is considered a low dose of steroids (less than 8 mg), many of these physical changes gradually lessen or disappear.
What can you do?
You can focus on the amazing things your body is doing as it fights this battle against vasculitis. Have compassion for yourself, just like you would for someone who is experiencing appearance changes as a result of medical treatments such as chemotherapy or because of a disease such as vitiligo. Talk to yourself the way you would talk to a friend or loved one if they were going through the same experience.
“It is really important to understand that the way that prednisone works metabolically inside your body weight gain is a very common side effect. You can do all the right things, you can eat all the right foods, you can exercise, and you can still have this side effect. This blame of the patient we really have to stop doing because it truly is a side effect of the medication. It’s kind of like blaming someone for losing hair when they take methotrexate.” – Dr. Catherine Sims, Rheumatologist
Possible Side Effects:
- Muscle wasting: weakening, shrinking, and loss of muscle
- Myalgia (muscle aches & pain)
It Worked for Us
We asked people who are living with vasculitis their best tips for dealing with muscle aches and pains. Here are some of their responses:
- Yoga and stretching
- Keeping hydrated
- Magnesium supplements
- Going for a short walk
- CBD oil cream
*Consult with your healthcare provider before adding any supplements or creams to your treatment plan.
Steps you can take to protect your muscles:
- Eat a diet with adequate protein, vitamins, and minerals
- Consider meeting with a registered dietitian
- Exercise, especially strength training, as tolerated
Try these simple strength training routines developed by fitness experts who have also been diagnosed with vasculitis.
Video: Seated Flexibility
Video: Beginner Seated Strength
Possible Side Effects:
- Thinning hair or changes in hair texture
- Thinning of the skin & skin tears
- Redness of the face (plethora)
- Stretch marks (striae)
- Steroid acne
- Increased facial hair
- Dark discoloration of the skin in body folds and creases (acanthosis nigricans)

What can you do?
- Use topical anti-acne medications
- Avoid sunburn
- Use a non-comedogenic (non-pore clogging) sunscreen
- Use vitamin E oil on stretch marks
- Use gentle chemical hair removers on excess facial hair
Possible Side Effects: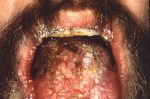
- Ulcers
- Thrush – overgrowth of fungus often first noticed as a whitish coating in your mouth and on your tongue
- Inflammation of the pancreas (pancreatitis)
- Inflammation of the stomach lining (gastritis)
- Stomach irritation-upset stomach, heart burn
- Increase in dental issues such as cavities and inflamed gums (gingivitis)
What can you do?
- Brush and floss regularly
Some dentists recommend using a water flosser - See your dentist at least four times a year so you can catch problems early
- Let your dentist know you are on a high-dose steroid treatment
Steps you can take to prevent stomach irritation:
- Take your steroid medication with food.
- Ask your healthcare provider about prescribing a medication that can help protect your stomach. Some of these medications cut down on the amount of stomach acid, some block the release of stomach acid, and some coat the stomach to help prevent irritation.
- Ask your healthcare provider if an over-the-counter antacid or other medication would help.
It is important to consult with your healthcare provider, even if you purchase an over-the-counter product, as antacids and other medications can impact the effectiveness of other medications you are taking, including steroids. Often it is just a question of timing when you take your prescribed medications and the antacid but be sure to discuss the timing with your healthcare provider and/or pharmacist.
How to treat thrush: If you suspect thrush, contact your healthcare provider, who can prescribe a medicated mouthwash or lozenges such as nystatin. There are over-the-counter mouthwashes for thrush, but nystatin is specifically designed for people with weakened immune systems and is only available by prescription. Depending on your medical history, some healthcare providers may prescribe a nystatin product to use to prevent thrush (prophylactic) when you begin your steroid treatment.
Possible Side Effects:
- Osteoporosis
- Avascular necrosis of the bone
- Decreased bone density and strength, which can increase your risk of bone fractures
Steps you can take to protect your bones:
- Work with your healthcare provider to get a baseline assessment of your bone health when you begin treatment with high-dose glucocorticoids (steroids). This may include imaging tests such as x-rays of your lateral spine or a DEXA scan.
- Address risk factors for osteoporosis that are in your control:
- If you smoke, quit.
- Add some simple weight-bearing exercises to your routine such as walking, wall or counter push-ups, and heel drops.
- Make sure you are getting adequate nutrition.
- Increase your intake of foods that are high in calcium and vitamin D.
- Limit your consumption of alcohol.
- Ask your healthcare provider about taking vitamin D and calcium supplements.
- Depending on your gender, age, and other risk factors, your healthcare provider may suggest additional measures such as taking certain medications that can help to reduce bone loss. You and your healthcare provider may find the American College of Rheumatology guidelines for the prevention and treatment of glucocorticoid-induced osteoporosis to be a useful resource.
Possible Side Effects:
- Cataracts
- Glaucoma: increased pressure in the eye (intraocular pressure)

- Exophthalmos: eyeballs might begin to protrude or bulge
Steps you can take to protect your eyes:
- Schedule an exam with an ophthalmologist (eye doctor) when you begin glucocorticoid (steroid) treatment.
- See your ophthalmologist at least once a year.
Interested in Learning More?
Possible Side Effects:
- More likely to develop upper respiratory tract infections and pneumonia
- Some white blood cells (part of the body’s immune system) will increase while others will decrease
- May take longer to recover from illnesses
- Wounds and infections may take longer to heal
- Increased susceptibility to other types of infections such as soft tissue infections and urinary tract infections
Why does this happen?
You are being treated with high doses of steroids to suppress your inflammatory response to reduce the inflammation of your blood vessels. While steroids are very effective at reducing the inflammation, they also suppress other aspects of your immune response, making it more difficult for your body to fight off infection.
What can you do?
- Though this may seem counterintuitive since steroids suppress your immune system, do not stop taking steroids while fighting an infection. If you are in the process of tapering and become ill, your healthcare provider may recommend that you temporarily suspend the taper as your body needs steroids during infection. (This is connected to the effects of high-dose steroids on your adrenal glands.)
- Depending on the treatments you are receiving, your doctor might put you on a prophylactic (preventive) antibiotic to reduce your chances of getting certain lung infections that are more common in people who are on high-dose steroids.
- Keep doing the basics: Sanitize high-touch surfaces, wash your hands frequently, avoid touching your face, keep your distance, and avoid crowded places.
- Give your body the nutrients it needs.
- Ask your healthcare provider whether or not they suggest you get a tuberculosis (TB) test and a blood test to see whether you have antibodies against certain viral infections such as chickenpox. TB may not show up in testing once a person has begun high-dose steroid treatment, so it is important to know whether or not you have TB before treatment. You are also more susceptible to certain infections such as chickenpox and these infections are more dangerous for someone who is on high-dose steroid treatment, so it is important to know if you already have some immunity to these infections.
- Make sure you are up to date on all of your vaccinations, including the shingles vaccine if applicable.
- There have been occasional reports of people experiencing their heart beating with an abnormal or irregular rhythm (arrhythmias). This is rare. People who are receiving high-dose intravenous glucocorticoids (steroids) are at the most risk. You will be in the hospital while receiving high-dose IV steroids and will be monitored for this possible complication.
- Some people experience an increase in the amount of fat in their bloodstream (dyslipidemia), changes in the balance of good and bad fats in their body, and an increase in the amount of fatty material that accumulates on the inner walls of their arteries (atherosclerosis). Your healthcare provider will monitor these levels with blood tests and may prescribe medications. Making dietary changes such as following a Mediterranean style diet and adding cardiovascular exercise such as walking as tolerated can also help.
Most people on high-dose glucocorticoids (steroids) will notice an increase in their blood pressure. In some people the blood pressure increases to the point that they are considered to have high blood pressure (hypertension.) If this occurs, your healthcare provider may prescribe medications to help lower your blood pressure. You can help decrease your risk of developing hypertension while on steroids by limiting the amount of salt in your diet, reducing stress, and exercising as tolerated.
Steroids significantly impact how your body processes sugar. If you already have diabetes, you will probably need to work with your healthcare provider to make adjustments to the medications you are taking for diabetes to make sure you keep your blood sugar levels are controlled.
If you don’t have diabetes, steroids may lead to the development of diabetes. You can reduce your chances of developing diabetes by:
- Limiting the amount of sugar in your diet, including the sugar from simple carbohydrates such as white bread, white rice, and potatoes
- Exercising as tolerated
- Meeting with a nutritionist or dietician who specializes in diabetes management
- Eating foods that are low on the glycemic index scale
Additional Resources
Websites
Books & Articles
- Coping with Prednisone by Eugenia Zukerman and Julie R. Ingelfinger, M.D.
- A practical guide to the monitoring and management of the complications of systemic corticosteroid therapy
Don’t Get Discouraged
“I used to think having to bump up prednisone was an admittance of failure. Just understand that’s not really the case. Don’t get discouraged because you have to go back up on your prednisone dose. Know that we’ve all been there.”
-Ben Wilson, Sports Broadcaster | Diagnosed with EPGA in 2014