VPPRN Patient-Powered Research
Our Research Discoveries
The VPPRN Research Team is relentlessly exploring every aspect of vasculitis — from the journey to diagnosis to quality of life to clinical trials of new treatments and population-wide studies of the disease. Our core mission is to translate this knowledge into new strategies to improve the lives of patients. Our Research Teams are making scientific progress and gaining an improved understanding of vasculitis.
None of this could be accomplished without our patient community. Thank YOU to all of our participants for making these research discoveries possible.
Below are some of our VPPRN discoveries and advances in vasculitis research and understanding. Keep checking back for new updates and study summaries.

VPPRN Poster Gallery | Research in Action
For our latest research results, check out our VPPRN poster gallery!
VPPRN Community Dashboard
See how you compare with others in the VPPRN community!
VPPRN Publications and Research Discoveries
VascSkin: Skin Vasculitis Quality of Life Survey, May 2023
 Skin involvement caused by vasculitis can be painful, burning, itching, and visible to others. Their impact on quality of life and well-being can be serious and is poorly understood by direct care providers.
Skin involvement caused by vasculitis can be painful, burning, itching, and visible to others. Their impact on quality of life and well-being can be serious and is poorly understood by direct care providers.
Dr. Robert Micheletti, assistant professor of dermatology at the Hospital of the University of Pennsylvania, in partnership with the Vasculitis Patient-Powered Research Network (VPPRN), launched the VascSkin Study to better understand the impact of vasculitis-related skin involvement on patients’ quality of life.
190 adult patients in the VPPRN participated in this study. Based on the data collected using the Effects of Skin Disease on Quality of Life Survey (Skindex-29) and patient-reported data collected online from the VPPRN, we found that patients with skin manifestations of vasculitis have reduced scores in several measures of quality of life. These results suggest that skin vasculitis has a significant impact on health and well-being and a substantial impact on patients’ symptoms and self-perception of health.
Journey to Diagnosis, April 2021
Journey to Diagnosis: Diagnostic delays in vasculitis and factors associated with time to diagnosis
This study originated as a research suggestion and highest priority by the Vasculitis Patient-Powered Research Network’s (VPPRN) patient-partners. This patient-driven study is a shining example of the power of patients collaborating with clinicians to conduct meaningful vasculitis research. Patients with vasculitis encounter delays in obtaining an accurate diagnosis which can lead to substantial morbidity and increased mortality. This study sought to describe the diagnostic journey of patients with vasculitis and identify factors associated with time to diagnosis.
You can read the full study manuscript in the Orphanet Journal of Rare Diseases: https://ojrd.biomedcentral.com/articles/10.1186/s13023-021-01794-5
Accuracy of Self-Reported Diagnosis of AAV, July 2020
 Accuracy of Self-Reported Diagnosis of Antineutrophil Cytoplasmic Antibody-Associated Vasculitis
Accuracy of Self-Reported Diagnosis of Antineutrophil Cytoplasmic Antibody-Associated Vasculitis
To determine the reliability of self-reported diagnosis of antineutrophil cytoplasmic antibody (ANCA)-associated vasculitis: granulomatosis with polyangiitis (GPA), microscopic polyangiitis (MPA), and eosinophilic granulomatosis with polyangiitis (EGPA) from a large, international, internet-based cohort.
Patient self-report of a diagnosis of ANCA-associated vasculitis is reliable with 86-96% of patients fulfilling the ACR criteria or CHCC definitions for their disease. Additional confirmation of the findings using medical records is currently underway. These results strongly support the reliability of using online, patient-generated data for clinical and epidemiological research in ANCA-associated vasculitis.
Developing Methods to Link Patient Records across Data Sets that Preserve Patient Privacy, May 2020
 Data from healthcare systems, patients and communities, and health plans can support health research. Two types of data sources are:
Data from healthcare systems, patients and communities, and health plans can support health research. Two types of data sources are:
- Patient-powered research networks, or PPRNs. In PPRNs, patients, families, caregivers, and community members share health data with the network. They work closely with researchers to plan and conduct research.
- Health plan research networks, or HPRNs. In HPRNs, networks of health plans have access to health claims data from members for research.
To link records, researchers use computer programs to connect the records of people in a PPRN with their claims data in an HPRN. Current methods to link records require use of personal information, such as names and dates of birth. But patients may not want to share this information. In this project, the research team developed method for linking data from PPRNs and HPRNs without using patients’ personal information.
the vasculitis pregnancy registry (VPREG): baseline information, march 2019
 The Vasculitis Pregnancy Registry (VPREG): baseline information for the first 3 years
The Vasculitis Pregnancy Registry (VPREG): baseline information for the first 3 years
The Vasculitis Pregnancy Registry (VPREG) is an online, patient-driven prospective pregnancy registry that is designed to collect observational data to increase our understanding of pregnancies in women with vasculitis.
Between 11/2015-12/2018 62 pregnant women with a range of vasculitis diagnoses enrolled in VPREG. Almost all (95%) had been diagnosed with vasculitis prior to conception and 67% had been hospitalized for vasculitis at some point.
comparison of patient self-reported data to physician-driven cohorts, november 2019
 Comparison of Patient Self-reported Data to Physician-driven Cohorts in Patients with Eosinophilic Granulomatosis with Polyangiitis
Comparison of Patient Self-reported Data to Physician-driven Cohorts in Patients with Eosinophilic Granulomatosis with Polyangiitis
Aligning views of patients and physicians in the diagnosis and management of diseases is imperative, particularly in rare, chronic diseases such as vasculitis. The aim of this study was to compare the patient-reported vs. physician-reported symptoms, treatments, and outcomes in patients with eosinophilic granulomatosis with polyangiitis (EGPA).
journey to diagnosis, november 2019
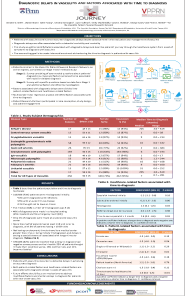 Diagnostic delays in vasculitis and factors associated with time to diagnosis
Diagnostic delays in vasculitis and factors associated with time to diagnosis
This patient-centric study of patients with vasculitis demonstrated that misdiagnosis and delays in diagnosis of vasculitis are quite common and identified several important clinical and health system factors associated with delays in diagnosis. The results of this study could lead to improved strategies to address diagnostic delays in vasculitis.
the cumulative burden of damage for patients with EGPA, November 2019
 The Cumulative Burden of Damage for Patients with Eosinophilic Granulomatosis with Polyangiitis
The Cumulative Burden of Damage for Patients with Eosinophilic Granulomatosis with Polyangiitis
This study aimed at describing damage in patients with EGPA enrolled in the Vasculitis Clinical Research Consortium (VCRC) from 2003 – 2019. The term “damage” in this study means any aspect of chronic disease that cannot be reversed with therapy.
Patients with EGPA endure considerable damage from the disease and disease treatment, even several years after diagnosis. The data shows the significant need for finding more effective and safer treatments for EGPA, especially those that limit the use of steroids.
patient involvement in medical research: what patients and physicians learn from each other, january 2019
 This project examined the recently formed Vasculitis Patient-Powered Research Network (VPPRN) to better understand what investigators and patients learned from working on research teams together.
This project examined the recently formed Vasculitis Patient-Powered Research Network (VPPRN) to better understand what investigators and patients learned from working on research teams together.
Direct engagement in research design and development by patient- partners and co-learning between investigators and patient-partners can result in a positive and productive working relationship for all members of a medical research team. This bi-directional engagement directly benefits and impacts research design, participant recruitment to studies, and study subject retention.
validation of the AAV patient-reported outcomes (AAV-PRO), april 2018
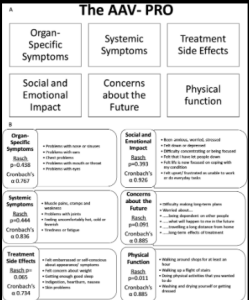 Validation of the ANCA-associated vasculitis patient-reported outcomes (AAV-PRO) questionnaire
Validation of the ANCA-associated vasculitis patient-reported outcomes (AAV-PRO) questionnaire
Developed and validated a questionnaire to assess quality of life in patients with ANCA-associated vasculitis (AAV). Patients with AAV have inflammation in the small blood vessels leading to involvement of a range of organs, for example kidneys, lungs and skin. Patients can suffer from ongoing disease activity or treatment side effects.
Quality of life can be measured by patient reported outcome measures (PROMs). This project developed a disease specific PROM for patients with AAV.
vascWork study: impact of vasculitis on employment and income, june 2018
 VASCWORK STUDY: IMPACT OF VASCULITIS ON EMPLOYMENT AND INCOME: AN ONLINE SURVEY OF PARTICIPANTS IN THE RARE DISEASES CLINICAL RESEARCH NETWORK – VASCULITIS CLINICAL RESEARCH CONSORTIUM PATIENT CONTACT REGISTRY
VASCWORK STUDY: IMPACT OF VASCULITIS ON EMPLOYMENT AND INCOME: AN ONLINE SURVEY OF PARTICIPANTS IN THE RARE DISEASES CLINICAL RESEARCH NETWORK – VASCULITIS CLINICAL RESEARCH CONSORTIUM PATIENT CONTACT REGISTRY
Work disability associated with rheumatic diseases accounts for a substantial financial burden. However, few studies have investigated disability among patients with vasculitis.
The purpose of this study was to examine the impact of vasculitis on patient employment and income.
development of case-finding algorithms for identifying patients with AAV, november 2016
 DEVELOPMENT AND VALIDATION OF CASE-FINDING ALGORITHMS FOR THE IDENTIFICATION OF PATIENTS WITH ANTI-NEUTROPHIL CYTOPLASMIC ANTIBODY-ASSOCIATED VASCULITIS IN LARGE HEALTHCARE ADMINISTRATIVE DATABASES
DEVELOPMENT AND VALIDATION OF CASE-FINDING ALGORITHMS FOR THE IDENTIFICATION OF PATIENTS WITH ANTI-NEUTROPHIL CYTOPLASMIC ANTIBODY-ASSOCIATED VASCULITIS IN LARGE HEALTHCARE ADMINISTRATIVE DATABASES
The aim of this study was to develop and validate case-finding algorithms for granulomatosis with polyangiitis (Wegener’s, GPA), microscopic polyangiitis (MPA), and eosinophilic GPA (Churg-Strauss, EGPA).
VPPRN and Autoimmune Research Collaborative (ARC) Publications
This article discusses the shared capacities and challenges of the Patient-Powered Research Networks (PPRNs) model, and the opportunities presented by collaborating across autoimmune conditions to design, conduct, and disseminate patient-centered outcomes research.
In this research article published in The Journal of Rheumatology, George et al, assess the concerns and healthcare-related behaviors of patients with autoimmune rheumatic diseases during the COVID-19 pandemic. Among 1,517 patients with different autoimmune conditions, disease-modifying anti-rheumatic drug (DMARD) use, and geographic measures of urban status, income, education, and COVID-19 activity, the authors found that patients with RA, PsA, AS, and SLE frequently avoided office visits and laboratory testing. Their findings highlight the need for adequate healthcare access and attention to vulnerable populations during the pandemic.
This study, conducted by Banerjee et al for the Vasculitis Patient-Powered Research Network, aimed to assess the concerns and health-related behaviors of patients with vasculitis during the COVID-19 pandemic. Survey responses from 662 patients demonstrated that during the early phases of the COVID-19 pandemic those with vasculitis had high levels of concern and exhibited potentially harmful health-related behaviors.
Throughout the course of the COVID-19 pandemic, assimilating and disseminating information has been challenging. In a recent review published in Current Opinions in Rheumatology, Duron et al evaluated threats to the validity of COVID-19 literature and proposed recommendations for rheumatologists and their patients. The authors note pandemic research exceptionalism and a parallel pandemic of misinformation as specific obstacles to finding high quality COVID-19 literature.
In a recent study, George et al compared the concerns and health-related behaviors of patients with autoimmune rheumatic disease with those who did not have non-autoimmune rheumatic conditions during the COVID-19 pandemic. 7176 patients with an autoimmune disease and 1828 patients without autoimmune diseases were included in this study based on completed surveys and meeting criteria for a primary diagnosis of interest. The authors found that patients with autoimmune rheumatic diseases had more concerns specific to their condition and were less likely to avoid office visits and testing during the COVID-19 pandemic.
Click here to read the full report and learn more about the findings.
The COVID-19 pandemic has had a major impact on healthcare, and the effect on rheumatology patients and providers is still unclear. In a recent study, Watrous et al look to understand the impact of COVID-19 on rheumatology office visits and parenteral immunosuppressive medications. The authors found the impact of COVID-19 on rheumatology office visits volume and immunosuppressive medications to be substantial, concluding that telemedicine and other tech focused healthcare tools are essential to optimizing rheumatology care and outcomes during the pandemic.
Those living with multiple sclerosis (MS) experienced changes in health behaviors and access to care due to the COVID-19 pandemic. However, the extent of the impact of the COVID-19 on this population has not been well characterized. In this cross-sectional survey of adults with MS registered in the iConquerMS platform, Vogel et al found that a majority of participants reported interruptions to their MS related care. Specifically, 64% of the 1,019 survey respondents canceled a medical visit, 22% canceled a neurologist visit, 11% canceled an MRI, 21% canceled a lab test, and 10% changed DMT in some way all due to COVID-19 related concerns or reasons.

